If your gynecologist has recently recommended minimally invasive gynecological surgery, you are probably wondering just what that entails. Most people are aware of the fact that any type of minimally invasive surgery is less invasive, which means it causes less trauma, uses smaller incisions, and has shorter recovery times than traditional open surgery. However beyond this, there are probably many things about minimally invasive gynecological surgery that you don’t know. In fact, one common thing that many women don’t know about minimally invasive gynecological surgery is that there are three different types, including:
Hysteroscopic Procedures
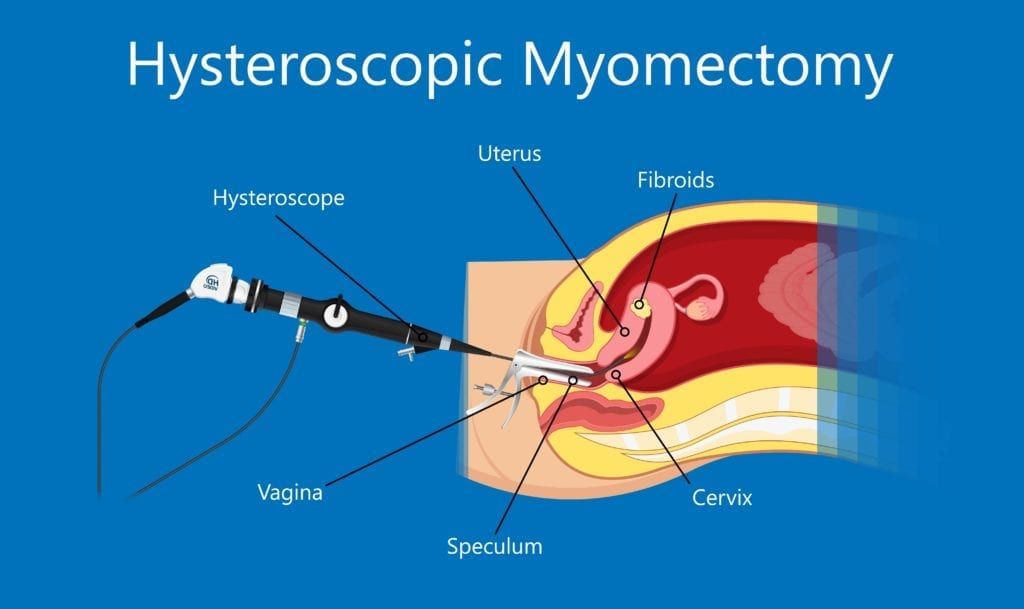
These procedures use a hysteroscope, which is a long, telescopic instrument that is inserted through the vagina and cervix until it reaches the uterus. Once in the uterus, the hysteroscope can be used to obtain magnified views of the uterus. Surgical instruments can also be passed through the hysteroscope in order to execute treatment.
Hysteroscopies are generally performed to explore the inside of your cervix and uterus when you are experiencing heavy menstrual bleeding and/or severe cramps, have had one or more miscarriages, or to diagnose fibroids, polyps, or scarring on the uterus. They can also be performed as a way to obtain a biopsy when you have an abnormal Pap result, as a sterilization procedure for permanent birth control, or to fix a misplaced IUD.
Laparoscopic Procedures
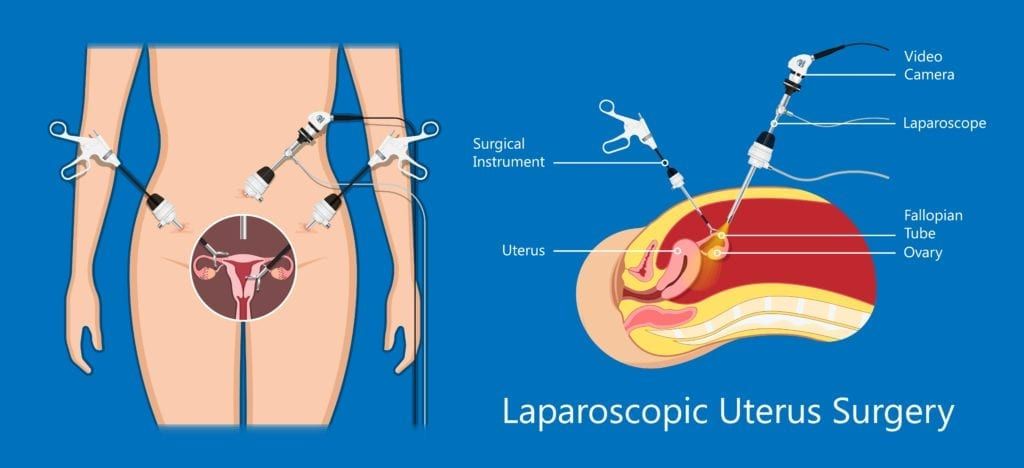
These procedures use a laparoscope, which is a long, telescopic instrument with a camera at the end, as well as 2 or 3 surgical instruments. The laparoscope is generally inserted through an incision in the belly button, while the surgical instruments are inserted through small incisions in the abdomen. The laparoscope provides a detailed video image of the surgical area, so that the surgeon can manipulate the surgical instruments as needed to complete the procedure. In the simplest sense, laparoscopic procedures are video-guided surgery.
Gynecological laparoscopic procedures can be used for diagnosis when you are experiencing pelvic pain or infertility. Gynecological laparoscopies can diagnose endometriosis, uterine fibroids, ovarian cysts or tumors, pelvic inflammatory disease, and reproductive cancers. Various treatments can also be administered using a laparoscopy, including: hysterectomy, endometrial tissue ablation, vault suspension for a prolapsed uterus, and the removal of ovarian cysts, fibroids, or the ovaries.
Robotic Procedures
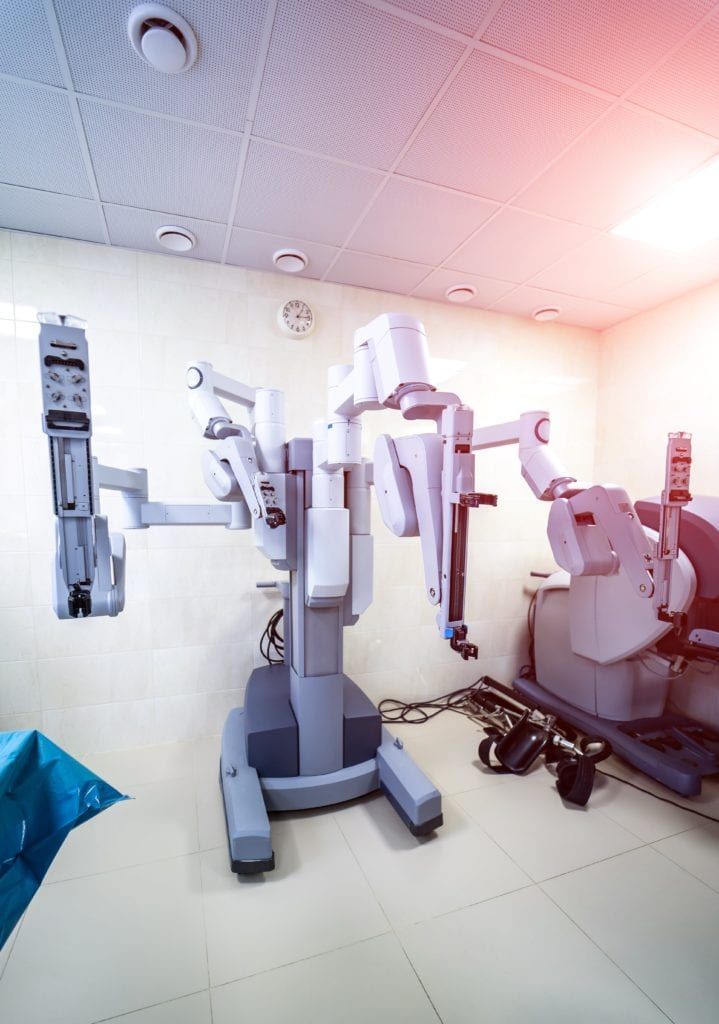
These procedures use a tool known as the da Vinci Surgical System. Like laparoscopic procedures, robotic procedures are video-guided and require multiple tiny incisions in the abdomen for a camera and surgical instruments. However the main difference between laparoscopic and robotic surgery is that the surgeon performs the surgery by controlling the surgical instruments and camera through a console located next to the patient.
Robotic procedures can be used to diagnose and treat the same conditions as laparoscopic procedures, however the difference is that these procedures are performed with the robotic surgical system. During your surgery, your surgeon will be able to view a highly detailed, magnified image of your anatomy and control tiny surgical instruments to complete the procedure. These instruments are designed to move like a human hand, but with a greater range of motion. This makes them ideal for precisely completing complex and delicate procedures.
As you can see, each of these minimally invasive gynecological surgical procedures has its own unique approach for diagnosing and treating specific gynecologic conditions. Ultimately, the type of minimally invasive surgical procedure your gynecologist will recommend depends on a number of factors. For this reason, it is recommended to discuss your options in greater detail with your gynecological surgeon before committing to surgery.

Dr. Geoffrey Zann is a Certified Robotic Da Vinci Surgeon, Board-certified by the American College of Obstetricians and Gynecologists, and a Diplomat of the American Board Obstetrics of Gynecology. He has been a member of the American Society for Colposcopy and Cervical Pathology, American Association of Gynecologic Laparoscopists, and the Hugh R. K. Barber Obstetric and Gynecologic Society.
