Did you know that it is recommended to have a well-woman examination performed every year in addition to your yearly physical? Just like an annual physical, these exams are used as preventative measures to maintain your health and screen for health issues that are exclusive to women. Your annual medical physical is intended to assess your overall health and are performed for both men and women. A well-woman visit, on the other hand, is a specialized examination that focuses on health issues exclusive to women. During a well-woman exam, your gynecologist will screen you for any abnormalities that warrant further testing. Therefore, it is important to have both a medical physical and a well-woman exam for a comprehensive assessment of your health.
During a well-woman exam one or more of the following may happen:
Discussion of Medical History
Before starting the exam, your gynecologist will ask you about your medical history, as well as your family’s medical history to determine if you may have an elevated risk for certain conditions. They will then ask you various questions about your reproductive and sexual health. These questions pertain to your periods, sexual activity, birth control, and any abnormal symptoms you may have experienced.
Breast Examination
Breast examinations start around age 25 and are usually every 1-3 years, depending on your age, as well as medical and family history. Since these examinations are used as early breast cancer screening tests, they will be performed more frequently if you or a close family member has been diagnosed with breast cancer, ovarian cancer, or if you are over the age of 40.
During a breast examination, your shirt and bra will be off so that your gynecologist can perform the exam. They will palpate your breasts with their fingers to look for lumps or abnormalities within the breast tissue. They will also look for abnormalities in your breasts size or shape, as well as in the texture of your skin. A breast exam will often conclude with your doctor showing you how to perform a self-examination and discussing what things to look for.
Pelvic Examination
Pelvic examinations start around age 21. How often you will need a pelvic exam will depend on your medical history. Generally speaking, you may need pelvic exams more often if you have a history of abnormal Pap test results or sexual health problems, have a family history of cancer, have or are seeing someone with an STD, or if you have recurrent vaginitis.
During a pelvic exam, you will be dressed in a paper or cloth gown. Your gynecologist will have you slide down to the end of the exam table and place your feet in stirrups to open your legs. While this may be an awkward position, it is the best position for performing the pelvic exam as comfortably as possible.
The first part of a pelvic exam is the external examination. During the external exam, your gynecologist will evaluate your vulva and the opening of your vagina for signs of cysts, discharge, warts, irritation, or other abnormalities. Next, they will perform a speculum exam of your internal structures. A speculum is a special tool made from metal or plastic that is inserted into your vagina and used to open the vagina so your gynecologist can examine it. It also allows your gynecologist to obtain a small sample of cells from your cervix, known as a Pap smear. This test screens for pre-cancer or cancer in the cervix.
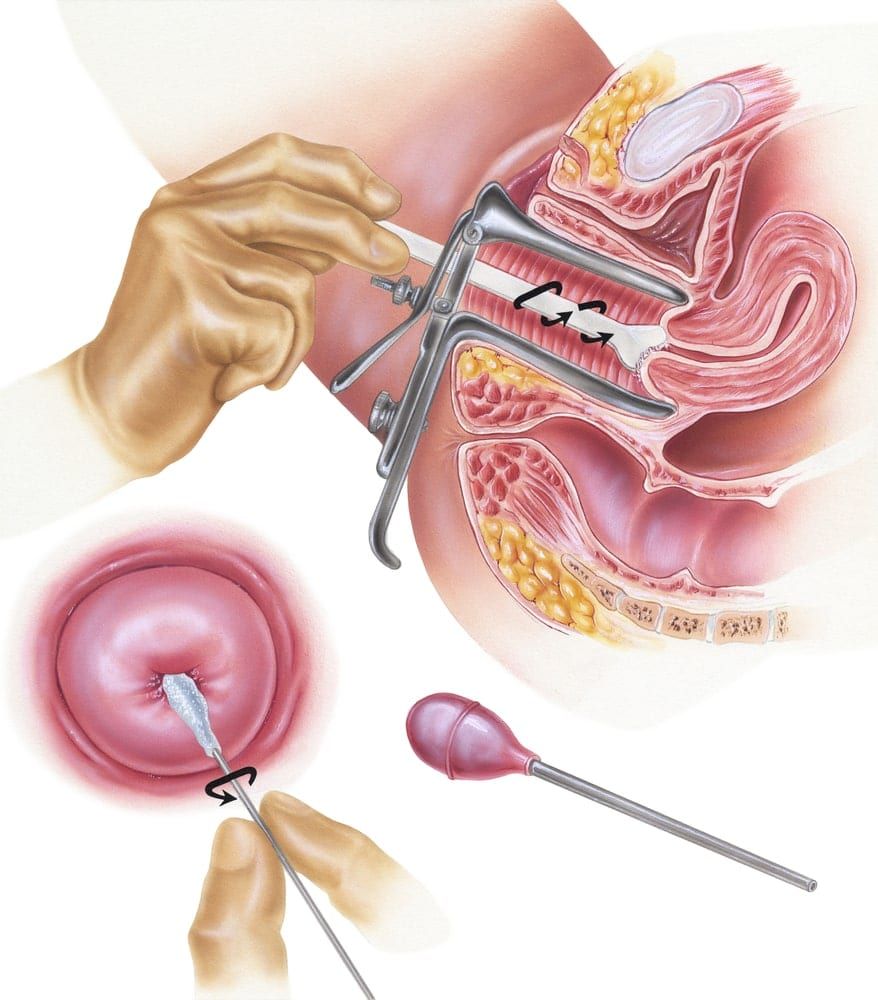
Next, your gynecologist will perform a bimanual exam by placing 1 or 2 fingers into your vagina and then using their other hand to apply gentle pressure on your abdomen. This exam allows them to feel the size, shape, and position of your uterus, as well as your ovaries and fallopian tubes. It also allows them to check for signs of tenderness, enlarged ovaries, ovarian cysts, or tumors. As a final step, your gynecologist may also perform a rectovaginal examination by placing one finger in your rectum and another in your vagina to check the muscles that sit between your vagina and anus. Finally, your gynecologist will answer any questions you may have before concluding the exam.

Dr. Geoffrey Zann is a Certified Robotic Da Vinci Surgeon, Board-certified by the American College of Obstetricians and Gynecologists, and a Diplomat of the American Board Obstetrics of Gynecology. He has been a member of the American Society for Colposcopy and Cervical Pathology, American Association of Gynecologic Laparoscopists, and the Hugh R. K. Barber Obstetric and Gynecologic Society.
